Message from the Chair

Dr. Richard G. Ellenbogen, Professor and Chair, Neurological Surgery
The Summer is a bittersweet time for me. It is a time we say goodbye to our beloved graduating Chief Residents who have served so brilliantly learning their craft, saving lives, writing papers/grants and training our students, junior residents and nurses. It is a time to reflect on their journey, character, perseverance and indomitable spirit during the first worldwide pandemic in a century. I am reminded how lucky we are to train these gifted and dedicated colleagues. In this edition, we review some provocative peer reviewed literature produced by our students and residents on ethnic medical disparities in our cancer patients and the diversity of our surgical house officers. There are faculty promotions, resident awards, NIH and Foundation Grants earned by our neurological surgeons and neuroscientists to celebrate. There are new Fellows, Faculty and Babies to herald in the most beautiful time in the Pacific Northwest, the spectacular summer season. And we Welcome our promising, talented young interns who we will surely celebrate when they graduate in 7 short years with their unique and equally impressive accomplishments. And the cycle of rebirth starts again! Thank you for Surviving, Thriving and Supporting our Mission to serve our patients and create a more promising future!
Very Respectfully,
Rich Ellenbogen
Special Announcement
Manuel J. Ferreira, MD, PhD named Chap and Eve Alvord and Elias Alvord Chair in Neuro-Oncology in Honor of Dr. and Mrs. Ellsworth C. Alvord, Jr.
The Alvord Family’s intention when they endowed this Chair was to recruit and retain distinguished faculty in neurological surgery. The Chap and Eve Alvord and Elias Alvord Chair in Neuro-Oncology in Honor of Dr. and Mrs. Ellsworth C. Alvord, Jr. Chair shall be filled by candidates who have achieved national recognition in the field of neurological surgery and who are expected to contribute to the advancement of teaching and research in their field.
This Chair is one of six honorary positions that helped to establish UW Medicine’s Nancy and Buster Alvord Brain Tumor Center, which is dedicated to the diagnosis and treatment of nervous system tumors. This endowment honors the late emeritus faculty member Dr. Ellsworth C. “Buster” Alvord, Jr., and his wife, Nancy D. Alvord. The Alvords and members of the extended Alvord family have shown tremendous dedication to UW Medicine with many gifs made to support research, faculty positions and patient care.
Dr. Ferreira is a nationally renowned talent in the treatment of skull base tumors through minimally invasive and novel endoscopic techniques. He has experienced a meteoric rise in our field to become a true “triple threat”. He is an NIH and Foundation-funded investigator researching the genomics of skull base tumors, Professor and the Chief of Neurological Surgery at the UWMC, Co-Director of the Alvord Brain Tumor Center, Co-Director of the Skull Base fellowship, and a Vice Chair of the Department of Neurological Surgery. He is beloved by his patients, a dedicated educator of residents and fellows, and meticulously runs one of the busiest tumor practices in the region. Dr. Ferreira is also the Clinical Director of the department’s Equity, Diversity and Inclusion efforts. Manny and his wife Anna are active in supporting the Seattle Community and are raising two wonderfully smart and athletic girls.
Buster and Nancy Alvord’s vision was always to create a world class destination center for patients with brain tumors, which also provided bench to bedside advancements in the novel treatment of these deadly and all too common tumors. Thus, there could be no better candidate than Dr. Ferreira for this illustrious Chair.
Contributed by Rich Ellenbogen, MD
Research and Innovation

Photo credit: Piron Guillaume, Unsplash
Racial and Ethnic Disparities Among Children with Primary Central Nervous System Tumors in the US
For children, brain tumors are the second most common cancer and have the highest mortality. Even so, disparities in incidence, survival and health care access related to racial and ethnic differences are not well understood. University of Washington medical student Edwin Nieblas-Bedolla worked with one of our Neurological Surgery residents, John Williams, and a multidisciplinary team from the University of Washington and several US institutions, to conduct a meta-analysis of existing studies to identify potential differences related to race or ethnicity in primary CNS tumors in children. Overall, their results, published in Neuro-Oncology, suggest that “…studies observed a higher incidence of CNS tumors amount White and Asian children in addition to higher burden of disease, lower access to care, and lower survival among non-White children.” The authors emphasize the importance of better understanding how race, ethnicity and clinical care intersect, particularly given that pediatric CNS tumors comprise approximately 18% of new pediatric cancers. Read the article.
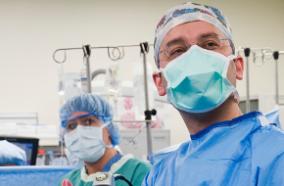
Photo credit: University of Washington Department of Neurological Surgery
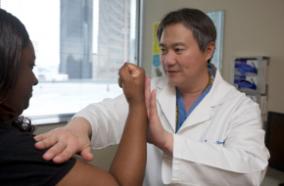
Trends in Race/Ethnicity Among Applicants and Matriculants of US Surgical Specialties, 2010-2018
In another report with University of Washington medical student Edwin Nieblas-Bedolla as lead author, published in JAMA Network Open, a multidisciplinary team including resident John Williams, examined trends from 2010-2018 in the percentage of applicants and matriculants to US surgical specialties identifying as members of an underrepresented racial/ethnic minority. The authors were interested in whether initiatives to improve racial/ethnic diversity have translated to increases in diversity of surgery program applicants or matriculants. Their analysis of data obtained from the Association of American Medical Colleges for 8 surgical specialties, including neurological surgery, found no overall change in underrepresented racial/ethnic minorities in these specialties during this time frame, suggesting that after earlier increases in racial/ethnic minority representation in surgical specialties in the 1990s and early 2000s, the representation of underrepresented minorities in these surgical specialties has plateaued. Indeed, the authors report a plateau affecting the entire training pathway from medical school applicants through practicing surgeons. Given this persistence through the training experience, the authors suggest reevaluating current strategies directed toward increasing racial/ethnic representation in surgery. Read the article.
Education
Graduating Residents’ Parting Thoughts

Ariana Barkley, MD
On Knowing Yourself
Constant evolution through this residency makes is such that “you” may become a fluid concept that is sculpted by lessons from each element of critique or praise; don’t forget to anchor this to your core values. Hold on to the people who center you and stay true to the “why” that drew you to neurosurgery in the first place. Try not to lose sight of your unique interests and continue to pursue them throughout residency; they may very well define your impacts in the field. In pursuing my global health interests, I observed what I take to be an inherent truth; aside from each person’s unique spark and particularities of circumstance, we are more alike than dissimilar. If nothing else, try to remember not to lose touch with your humanity during this process and that the pursuit of excellence in our field means taking care of the whole patient, their family and each other in addition to technical mastery.
Watch the 2021 graduation talks here.

Samuel Emerson, MD, PhD
Hike to the Heavens, A Metaphor for Neurosurgery Residency
Dr. Kim’s annual Hike to the Heavens is a good metaphor for neurosurgery residency in general. It’s long, difficulty, and you have to do it on very little sleep. At many points you wonder what the heck you were thinking. But it pays off with some really incredible sights and experiences that you really couldn’t get without all the pain invested. I really think about different sections of it as kind of the different years of residency. You start off full of optimism and feeling like you have this going and it’s up hill from the get go but you feel like you can do this. Very quickly you realize “this never stops” and perhaps you got more than you bargained for. Then you get up to the first break point where you get your first views and you have lunch, and that is like the end of R2 year, where you feel like you accomplished something, things have paid off, you’ve made it. But then you realize you can’t quite take your foot off the gas just yet because there is more climbing to do and you have another hour or two before you get up to the main ridge where the big views happen. Then you are up on this ledge for a good long hour where the sun is out now and there is total exposure and you feel like you are in this never-ending state of heat and pain and like it is never going to end, but eventually you come back down the hill and get to the lake. This is like R5 year where you get your energy and wind back. The last mile is like the chief years, where the end is in sight and the payoff is the best beer you’ve ever had in your life.
Watch the 2021 graduation talks here.

Jake Ruzevick
Advice to Junior Residents and Medical Students Considering a Neurological Surgery Residency:
Becoming a strong resident starts with 10 things that require absolutely no talent whatsoever, but that a lot of us seem to forget from time to time. When you feel like you are falling behind, hit the reset button and try to do these 10 things really well and you will find your path again.
TEN THINGS THAT REQUIRE ZERO TALENT
- Being on time
- Making an effort
- Being high energy
- Having a positive attitude
- Being passionate
- Using good body language
- Being coachable
- Doing a little extra
- Being prepared
- Having a strong work ethic
Resident News
Grants Received

Association of VA Surgeons Foundation, $25,000

SNIS Foundation, $25,000
Presentations
Residents had 12 abstracts accepted to the AANS Annual meeting in Orlando, Florida in August 2021.
Ariana Barkley, graduate: Acute postoperative seizures after laser ablation
Jessica Eaton, PGY-4: 1) Extra-arachnoid SDH and outcome; 2) Outcomes and complications related to timing of cranioplasty for TBI patients
Abdullah Feroze, PGY-7: Cellular Allograft for Stand-Alone Multi-Level Anterior Cervical Discectomy and Fusion
Maddie Greil, PGY-5: Posterior Fusion Across the Cervicothoracic Junction: Does Ending at T1 versus T2 Impact Outcome?
Jake Ruzevick, graduate: 1) Genotype of skull base meningiomas; 2) The retrolabyrinthine presigmoid approach: outcomes, techniques and operative pearls from 92 consecutive cases of petroclival and cp angle tumors
Rajeev Sen, PGY-5: 1) Concurrent Decompression and Resection of Ruptured Brain Arteriovenous Malformations in Clinically Unstable Patients; 2) Intraoperative Neuromonitoring for Pediatric Chiari Decompression: When should we use it?
Sanan Sivakanthan, PGY-5: 1) Early experience in endoscopic spine; 2) Economic impact of COVID-19 on high volume neurosurgical practice
New Residents
 .
.
Eliza Baird-Daniel, MD (left)
Originally from Seattle, Eliza attended Cornell University graduating cum laude with a BA in Neurobiology and Animal Behavior. Following graduation, Eliza spent two years as a research assistant at Weill Cornell Medicine’s Department of Neurosurgery under Dr. Theodore Schwartz where she designed and performed experiments investigating the spatiotemporal dynamics of seizure onset and spread and role of optogenetic inhibition in seizure control. Eliza was then accepted to the University of Colorado School of Medicine, where for 3 years she served as co-president of weekly student-run primary care clinics for residents of the Warren Village low-income housing community which serves approximately 200 single-parent families in Denver demonstrating her commitment to both peer and community health-literacy education. Working with the anatomy department to use human specimens to illustrate neuroanatomy and basic neuroscience principles, Eliza has further contributed to community health and science literacy as a co-creator of a “Neuroscience Patch” attainable by Girl Scout troops in the Denver metro area. The honors she has achieved over the past 4 years include the Luis and Rachel Rudin Foundation Diversity Scholarship, the University of Colorado Student Research Forum Top Poster Award and the Mike Carry Fund Scholarship Recipient. Eliza was also recognized for her academic and leadership excellence with selection to the University of Colorado AOA.
Julian Clarke, MS, MD (center)
Julian grew up in Toronto, Canada, where he excelled both academically and athletically. He represented Canada at the World Cup competition for basketball, which led to a career as a Division 1 athlete at Santa Clara University. After earning his B.S. in Biochemistry, Julian pursued a Masters Degree in Exercise Science at the University of Toronto and was then accepted at Washington University School of Medicine. Very early on, Julian distinguished himself as a student having serious interest in neurosurgery and in basic research. He completed a 2-year research fellowship in Dr. Gregory Zipfel’s lab where he pursued fundamental experiments examining the impact of subarachnoid hemorrhage on the neurovascular unit utilizing novel optical imaging techniques to measure functional connectivity in collaboration with Dr. Joe Culver. He was awarded the Washington University Dean’s Fellowship for Research and the Mound City Medical Forum Scholarship. In his free time, Julian volunteered as a basketball coach and mentor at Clayton High School in St. Louis.
Katherine Kelly, MD (right)
A native of Tennessee, Katherine attended Northwestern University where she earned her BA in Cognitive Neuroscience and was a member of the University’s varsity sailing team. She returned to Tennessee to undergo her medical training at Vanderbilt University’s School of Medicine. Katherine has a particular passion for surgical outcomes and health disparities research and has led several projects which helped change the educational process for primary care practitioners to better recognize craniosynostosis in lower socioeconomic communities of Tennessee. For her efforts, Katherine has a robust CV with 9 peer-reviewed manuscripts, including several first-author, and over 20 presentations at national and regional meetings. An effective leader, Katherine served as president of the Neurosurgery Careers in Medicine group, secretary of the American Association of Neurological Surgeons, and mentorship chair of the Association of Women Surgeons, helping to guide underrepresented students, particularly women, to pursue a career in neurological surgery. As a 3rd-year medical student, Katherine traveled to Zambia to work alongside the local neurosurgery team. During this time, she worked in a hospital with limited access to water and electricity to help care for underserved patients suffering from many neurosurgical problems including tumors and spina bifida. In addition to her MD degree, Katherine pursued a Health Equities Certificate to better understand both local and global challenges to public health.
People
Special Announcement

Tram Tran, MPA
Associate Director, Neurological Surgery and Neurology
Congratulations to Tram Tran, who in June logged 25 years of service to the University of Washington! The Department of Neurological Surgery greatly appreciates her dedication to our Department and to UW Medicine!
Promotions

Professor of Neurological Surgery

Clinical Associate Professor of Neurological Surgery
Grants Received

National Institutes of Health, $95,149

Measurement and Modulation of Neural Activity in Brain Cancer
Wayne D. Kuni & Joan E. Kuni Foundation, $75,000

Defining Cellular States of Quiescence in Human Brain Tumors
National Institutes of Health, $600,000

Automated Optimization of Adaptive DBS for Parkinson’s Disease
Weill Neurohub Research Award, $280,373

Christoph P. Hofstetter, MD, PhD
Closed-loop Spinal Stimulation for Restoration of Upper Extremity Function After Spinal Cord Injury
Department of Defense Congressionally Directed Medical Research Programs, $410,176

Richard G. Ellenbogen, MD and Manuel Ferreira, MD, PhD
Wayne D. Kuni & Joan E. Kuni Foundation, $75,000
New Team Members

Acting Assistant Professor, Pediatric Neurosurgery
Acting Instructor, Epilepsy and Functional Neurosurgery

Acting Instructor, Cerebrovascular and Skull Base Fellow

Visiting Assistant Professor, Spine & Spinal Cord Injury

Acting Instructor, Spine Surgery Fellow

Acting Instructor, Pediatric Neurosurgery Fellow
Cormac Robert Bonow
Drs. Rob Bonow and Laura Spece welcomed Cormac Robert Bonow into the world on 7/2/2021. Cormac weighed 6lbs, 3oz at birth and measured 19.5 inches. Please welcome the newest member of our department, Cormac!