Message from the Chair


Dr. Richard G. Ellenbogen, Professor and Chair, Neurological Surgery
What a year it has been! Despite the COVID pandemic, our department has showed its indominable spirit and the best of its warm, supportive culture. “Resilience” at this point is a term that frankly underestimates the performance by our faculty, residents, nurses, APP’s, administrative staff and students. When one of us went down from illness, another stepped in, without missing a step. We have been clinically more productive in the operating rooms and telemedicine clinics, garnered more grants, and kept the Neurological Surgery machine running by our able staff. This newsletter is just a sampling of the positive news earned by hard work, great ideas and a superb team spirit. I “thank you”, knowing that this phrase simply does not capture my abiding appreciation and admiration for each of you. Just know that I feel fortunate every day to work with you on the mission of this wonderful department.
Very Respectfully,
Rich Ellenbogen
Special Announcement
Christine Mac Donald, PhD named Vice Chair for Research, Department of Neurological Surgery
Christine Mac Donald, PhD, Professor and James and Gaye Pigott Endowed Chair, Research Director, The Sports Institute at UW Medicine was named the new Vice-Chair for Research, Department of Neurological Surgery. She assumes the position from Professor Jeff Ojemann, MD who has been elevated at Seattle Children’s Hospital to Chief Medical Officer and Senior Vice President.
Dr. Mac Donald is a phenomenon! She is currently the PI or investigator of 11 active extramural grants! This includes being PI on 2 R01s from NIH and multiple NIH, DOD and Foundation grants. She is successful because of her wonderful combination of innovative new ideas, a tireless work ethic, and an unparalleled collaborative spirit. She has had a meteoric career since she arrived at UW and is recognized by residents, faculty and students as one of the thought leaders in our department. She has played an instrumental role in our R-25 training grant with underrepresented minority college students in inspiring them to pursue careers in science and medicine. I am thrilled she has accepted her new position.
Contributed by Rich Ellenbogen, MD
Patient Care

Seattle Magazine Top Doctors 2021
Congratulations to members of the department who were voted the Top Doctors in Seattle for 2021 by Seattle Magazine. For more than two decades, Seattle magazine has published a list of the region’s top doctors, all of whom were nominated by their peers. A total of 8 neurosurgeons, 4 pediatric neurosurgeons, and 2 of the department’s physician assistants made the list. Congratulations to Drs. Ellenbogen, Ferreira, Kim, Levitt, Patel, Ravanpay, Silbergeld, Zhang, Browd, Hauptman, Lee, Ojemann, and Young Cho and Alfred Noriega!
Research and Innovation
How Telemedicine in the Operating Room Will Transform Surgery
“Imagine the ability to take expert surgical knowledge and share it with colleagues and trainees anywhere in the world on-demand or real-time, live in the moment…” In this article, Dr. Sam Browd describes his experience virtually proctoring an Australian colleague through a selective dorsal rhizotomy and how he sees the potential for communications tools to democratize access to essential knowledge in neurological surgery. Read the article.
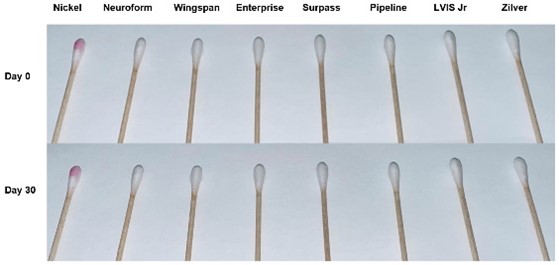
Nickels and Tines: The Myth of Nickel Allergy in Intracranial Stents
Congratulations to the Cerebrovascular Research Group and the Stroke & Applied Neuroscience Center (SANS) for their recent publication in the Journal of NeuroInterventional Surgery. The authors, including medical student Kevin Vanent, Emma Federico (SANS), residents David Bass and Guil Barros, Jade Keen (SANS), and lead faculty Mike Levitt, showed that nickel release from commonly used intracranial stents is negligible. The authors conclude that hypersensitivity to these stents may be misattributed to nickel allergy, and that patients with nickel allergy may be safely treated with select nickel-containing stents. Read the article.

Can an electroceutical treat rheumatoid arthritis?
Can nerve stimulation reduce the inflammation that causes rheumatoid arthritis? Dr. Andrew Ko is performing the surgeries for a study by UW Medicine physicians that aims at answering that question. A small electronic device, the size of a vitamin tablet, will placed around the left vagus nerve through an incision in the neck. Low voltage stimulation will be applied at night during sleep and after 12 weeks, the severity of rheumatoid arthritis will be assessed. Dr. Ko says: “…if this novel approach proves effective, it may work for other autoimmune diseases as well.” Read the article.
Residents News
Grants Received
Guilherme Barros, MD
Robert J. Dempsey, MD Cerebrovascular Resident Research Award, $15,000
Maggie McGrath, MD
Richard H. Adler Attorney at Law & Adler Giersch Law Firm Endowed Fund for Traumatic Brain Injury Research Award, $7500
Kate Carroll, MD
NIH R25, $95,139
Awards
Jessica Eaton, MD
Complications associated with early cranioplasty for patients with traumatic brain injury: a 25-year single-center analysis
Western Neurological Society Resident Award for Clinical Science
Presentations
Several resident research projects were accepted by the Western Neurological Society for their annual meeting in September 2021:
Jess Eaton, PGY 4: 1) Outcomes in Traumatic Brain Injury Patients with Purely Extra-Arachnoid Subdural Hematoma; 2) Complications Associated with Early Cranioplasty for Traumatic Brain Injury Patients: A 25-year Single-Center Analysis; 3) Cavernous sinus invasion as predictor for cure in pituitary adenoma patients with acromegaly
James Pan, PGY 4: Complications of Pediatric Tethered Cord Release: Seattle Children’s Hospital Experience
Guil Barros, PGY 5: Modeling the effect of hemodynamics on the endothelial cell transcription profile of cerebral aneurysms after endovascular flow diversion treatment
Abdullah Feroze, PGY 7: Cellular Allograft for Stand-Alone Multi-Level Anterior Cervical Discectomy and Fusion
Residents had 11 abstracts accepted to the CNS Annual Meeting in October 2021:
Malia McAvoy, PGY 2: 1) Low Allele Frequency Somatic Variants in Sporadic Saccular "Berry" Cerebral Aneurysms; 2) Somatic Mosaicism of a PDGFRB Activating Variants in Intracranial, Coronary, Aortic and Radial Vascular Beds
Scott Boop, PGY 3: Robot-assisted stereoelectroencephalography in young children: technical challenges and considerations
Evgeniya Tyrtova, PGY 3: Surgical outcomes in adult and pediatric craniopharyngiomas
Jess Eaton, PGY 4: 1) Outcomes in Traumatic Brain Injury Patients with Purely Extra-Arachnoid Subdural Hematoma; 2) Complications Associated with Early Cranioplasty for Traumatic Brain Injury Patients: A 25-year Single-Center Analysis; 3) Cavernous sinus invasion as predictor for cure in pituitary adenoma patients with acromegaly; 4) Tract disruption in patients with pure language SMA vs motor SMA
James Pan, PGY 4: Complications of Pediatric Tethered Cord Release: Seattle Children’s Hospital Experience
Dave Bass, PGY 6: Lagrangian particle tracking for coiled aneurysms
Mike Meyer, PGY 6: Penetrating trauma angio versus CTA
In addition, the following resident research was accepted to the Annual Meeting of the Society for Neuro-Oncology in November 2021:
Abdullah Feroze, PGY 7: A single-cell based precision medicine approach using glioblastoma patient-specific models
Resident research was also presented at the AANS/CNS Pediatrics Section Annual Meeting in December 2021:
Katherine Kelly, PGY 1: The role of traditional social determinants of health in referral patterns, timing of surgery, and CHIP-determined QOL in children with symptomatic Chiari I Malformation
People
Faculty awards
Western Neurological Society 2021 Cloward Award Recipient
Ralph Cloward: From Pearl Harbor to Renaissance Man and Pioneer in Spine Surgery
Faculty Grants and Contracts Received
Outcome pRognostication of Acute brain injury with the NeuroloGical pupil indEx - ORANGE, University of Milan, $1,499
Transforming Research and Clinical Knowledge in Traumatic Brain Injury Network (TRACK-TBI NET), University of California, San Francisco, $102,409
Pediatric Severe Traumatic Brain Injury in Latin America – A Randomized Trial Comparing Two Management Protocols, with Nancy R. Temkin PhD, Jim Pridgeon MHA, Robert H. Bonow MD, National Institutes of Health, $651,505
Brain Oxygen Optimization in Severe Traumatic Brain Injury—Phase 3 (BOOST-3)-CCC, with Nancy R. Temkin PhD, University of Michigan, Ann Arbor, $312,775
Summer Research Experience in Translational Neuroscience and Neurological Surgery, National Institute of Neurological Disorders and Stroke, National Institutes of Health, $103,919
Accelerating Dissemination of Implantable Neurotechnology for Clinical Research, University of California, San Francisco, $41,035
Early detrusor chemodenervation for preservation of bladder compliance and longevity after spinal cord injury, Craig H. Neilsen Foundation, $150,000
A Randomized, Sham-Controlled, Double-Blind Study of Vagus Nerve Stimulation for Moderate-to-Severe Rheumatoid Arthritis: The RESET-RA Study, SetPoint Medical, $163,290
Minimally Invasive IntRaceRebral HemORrhage Evacuation, Icahn School of Medicine at Mount Sinai, Integra Life Sciences Corporation, $17,399
Embolization of the Middle Meningeal Artery with ONYXTM Liquid Embolic System in the Treatment of Subacute and Chronic Subdural Hematoma Evacuation (EMBOLISE), Medtronic, $145,218
Improving the computational modeling of coiled cerebral aneurysms through synchrotron microtomography, National Institutes of Health, $296,180
Human brain tissue collection and preservation for cortical neuronal cell type classification, Allen Institute for Brain Science, $74,202
Neurosurgery research training in interdisciplinary neuroscience, National Institutes of Health, $255,773
Improving Patient Classification and Outcome Measurement in TBI, Medical College of Wisconsin, $37,545
Transforming Research and Clinical Knowledge in Traumatic Brain Injury (TRACK‐TBI Longitudinal), University of California, San Francisco, $13,561
Viral reactivation from ganglia in subarachnoid hemorrhage, National Institutes of Health, $77,750
Novel Analytical Methods for Characterization of Cerebral Thrombectomy Specimens, DePuy Synthes Orthopaedics, Inc., $56,539
Zero G and ICP: Invasive and noninvasive ICP Monitoring of Astronauts on the ISS, NASA, $126,681
New Team Members
Assistant Professor
Dr. Amin specializes in spine surgery with a focus on spinal oncology. He received his medical degree from the Johns Hopkins University School of Medicine, completed neurosurgery residency at New York Medical College at Westchester Medical Center, and a neurological oncology fellowship at Memorial Sloan Kettering Cancer Center.
Finally, please welcome these 3 smallest members of the Neurological Surgery family!

Ace Messod Abecassis
Sarah and Josh welcomed Ace on July 17, 2021. He was 9 lbs 6 oz at birth! Nuff said.

Axel Engstrom McGrath
Anika and Lynn welcomed Axel on Nov 3, 2021. He weighed in at 7 lbs 8 oz and is named after Anika’s great grandfather who was a Rough Rider with Teddy Roosevelt.

Lily Morenz Emerson
Grace and Sam welcomed Lily on Nov 10, 2021. She was 8 lbs 3 oz at birth; Grace and Sam “have been in a haze of snuggles and dirty diapers” since she was born.