Overview
The safety and effectiveness of surgery for acoustic neuromas has considerably improved during the past 10 years with the advent of specialized techniques in microsurgery, neuro-anesthesiology and intraoperative monitoring.
In addition to surgical treatment, therapy using stereotactic radiosurgery and nonsurgical monitoring of small tumors has provided new options in the treatment of these lesions.
The guiding philosophy at UW Medicine is to manage patients with acoustic neuromas without producing any new neurologic deficits. In some cases, this leads to early surgery to preserve hearing, and, in other cases, this means observing the tumors if surgery is more risky.
Treatment is individualized depending on the circumstances for each patient to assure the best outcome.
Preoperative testing
Each patient undergoes a multidisciplinary preoperative evaluation before acoustic neuroma treatment. The usual preoperative tests, including electrocardiogram, blood tests and chest X-ray, will be performed. The patient will also have the following studies:
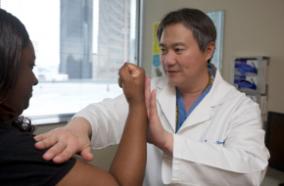
Audiogram
This measures the hearing capacity for both the affected and unaffected ears. This information guides the team in decisions about when to operate and whether hearing can be preserved.
Brainstem auditory evoked potential: This test measures the conduction of electrical signals along the cochlear, or hearing, nerve. This preoperative assessment is essential when hearing is present since this test is used during surgery to monitor the cochlear nerve in order to preserve hearing.
Vestibular testing
Vestibular, or balance, testing is done to determine the amount of loss of balance function of the inner ear from the tumor and the branch of the balance nerve being affected. Some patients have little loss of function and can expect to be quite dizzy after surgery. Others have already lost their balance function and have little difficulty.
The main vestibular test is the ENG, or electronystagmogram. It measures the function of the respective inner ear balance organs. Balance function is also measured with a posturography platform test. Not all patients undergo vestibular testing preoperatively. The test may help identify those patients who will require more aggressive vestibular rehabilitation therapy postoperatively.
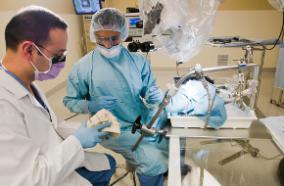
Surgical Approaches
At UW Medicine, neurosurgeons use three different surgical approaches to treat skull base tumors. Each has advantages and disadvantages and is individualized according to hearing level, size and location of the tumor and patient wishes.
Suboccipital approach
In this approach a window of bone is removed from the skull behind the mastoid. Gentle retraction of the cerebellum provides exposure of the tumor at the brain stem. Additional bone is removed overlying the posterior part of the internal auditory canal. This approach provides excellent exposure of the tumor and adjacent brain tissue and allows for hearing preservation. It may be used for small and large tumors.
In a retrospective review of almost 100 patients at the UW Medical Center, hearing was preserved in almost 70 percent of patients when the tumor size was less than 2 cm. The total length of the operation varies from 6 to 12 hours, depending upon the size of the tumor and whether it is attached to critical structures.
Translabyrinthine approach
The translabyrinthine approach was developed in the 1960s for use in patients with small- to medium-sized tumors in whom hearing function was absent or not useful. At that time, this approach was a great technical advance and substantially reduced the complication rate after surgery.
There are three technical advantages to the translabyrinthine approach: exposure, bone removal and identification of the facial nerve. By directing the surgical access through the mastoid bone and inner ear, or labyrinth, there is less need for retraction of the brain for exposure.
In addition, the bone dust from drilling is removed before the membrane surrounding the brain is opened, which decreases the amount of headache after surgery. Finally, the facial nerve is identified early in the case, which reduces the chance of injury. The major disadvantage of this technique is total deafness.
Middle fossa approach
In this approach a window of bone is removed from the skull above the ear. The brain is gently lifted from the skull base and the bone overlying the tumor in the internal auditory canal is removed from above. This approach is best suited for small tumors in ears with good hearing. When favorable preoperative conditions exist, hearing preservation rates may approach 80 percent. The major disadvantage is a higher incidence of temporary facial weakness.
Stereotactic radiosurgery
This is an outpatient, nonsurgical procedure in which a beam of high-dose radiation is focused on the tumor. The radiation may be delivered in a single dose or multiple (fractionated) doses. This delivery is intended to minimize injury to the surrounding nerves and brain tissue. Tumor growth ceases in more than 90 percent of patients and, in rare cases, the tumor may shrink. Initial hearing preservation rates have been high, but decline during time.