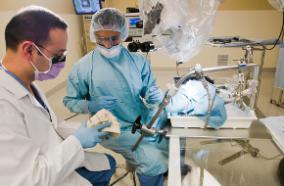
Deep brain stimulation (DBS) delivers an electrical current to small areas of brain tissue near the brainstem. This electrical current changes, or modulates, the communication between nerve cells in the brain.
The symptoms of disease, such as slowness of movement, stiffness or tremor, are caused by abnormal communication between nerve cells. Deep brain stimulation will silence this abnormal communication and restore function that is closer to normal. It is a standard surgical treatment for Parkinson’s disease, tremor and dystonia.
The electrical stimulation to the brain is delivered through a fine wire that is passed through brain tissue to reach a target deep in the brain. The wire extends to an implanted neurostimulator, or brain pacemaker, that is usually placed in the chest. The entire system is placed beneath the skin. The neurostimulator can be programmed to many different settings using a device that communicates with the neurostimulator through the skin.
Procedural Details
DBS surgery is usually divided into two stages. In stage one, the DBS leads (brain wires) are placed into the brain. In stage two, the neurostimulator device (brain pacemaker) is implanted and connected to the DBS leads with an extension wire.
Stage 1: DBS Lead Placement
In this stage, the DBS leads that deliver the electrical current are implanted.
- Patients need to be off all Parkinson’s disease medication for at least eight hours.
- Patients are wide-awake for most of the surgery, but may have mild sedation during certain times.
The success of DBS surgery depends on the accuracy of the placement of the DBS leads within a particular group of neurons (nucleus). Therefore, a stereotactic frame guides surgery. This metal frame is a highly accurate measurement device that is attached to a patient’s head like a halo. Using this frame, any location within the brain may be targeted precisely within a millimeter.
In order to match the frame with the patient’s brain, an MRI scan must be performed with this MRI-compatible frame in place. In addition, location of the DBS wires in the brain is confirmed with microelectrode recording and test stimulation. Microelectrode recording is essentially “listening” to the brain activity. Different areas in the brain have characteristic firing patterns, which means they sound differently when we listen to them.
Finally, when we are confident in the brain location, we perform a test to check for any side effects and benefits to the stimulation. After all this information is confirmed, the permanent DBS electrode is implanted in the brain, and the other end is tucked under the scalp for later connection to the neurostimulator. This procedure is usually performed on both sides of the brain during a single surgery.
Stage 2: Neurostimulator Implantation
In this stage, we connect the DBS brain electrodes to an implanted pulse generator or “pacemaker.”
This stage is an outpatient surgery that is scheduled one to three weeks after the first surgery. This surgery is performed under a general anesthesia. A stimulator device is typically implanted on each side of the upper chest so each of the two devices stimulate a side of the brain. It is possible to have a larger stimulator implanted only on one side that stimulates both sides of the brain. The decision between two smaller and one larger stimulator must be made before your first surgery.
Currently, the stimulators contain a non-rechargeable battery that must be replaced every four to five years. In the future, rechargeable batteries that are expected to last 10 years may be an option.
Medications
After DBS surgery, patients are often able to reduce their medications in consultation with their neurologist. Patients with Parkinson’s disease should never abruptly stop taking their medications.
Considerations
Patients with Parkinson’s disease, essential tremor or dystonia whose medications are not effective or causing side effects.
Effectiveness
This treatment is highly effective for certain movement related symptoms of Parkinson’s disease such as slow movement, stiffness and tremor. The treatment is highly effective for patients with tremor.
Risks
Major risks include bleeding in the brain, stroke, infection or incorrect placement of the DBS electrode. Life threatening risks are very rare, and this surgery is considered to be a safe, elective surgery. Other risks and side effects are associated with sedation and stimulation of the brain. Certain special precautions need to be taken after surgery.
For an explanation of risks, possible side effects and precautions, patients should speak with a neurosurgeon who practices this surgery or a movement disorders neurologist who is familiar with the surgery.
There are no risks for not having this procedure.
Urgency
This is an elective surgery, so there's no urgency in seeking treatment.